“The cartilage doc” – preserving joints instead of replacing them
Osteoarthritis
My basic treatment approach for osteoarthritis: preserve joints instead of replacing them
Osteoarthritis is the most widespread joint disease in the world. Sufferers feel pain, especially in the morning and during exertion. Sometimes the joints even make themselves felt at night. In X-rays and MRI scans, the protective cartilage becomes thinner or is completely missing. This objective “finding” does not necessarily correlate with the patient’s “complaints“. Orthopaedic surgeons should not treat images, but the complaints of their patients. The patient suffers above all when their osteoarthritis “activates“. This is the case when the joint becomes inflamed. Due to the inflammation, anti-inflammatory drugs such as cortisone, ibuprofen, diclofenac and similar medications also help in the short term. If you want to do something for your joint health in the long term, you need to treat the joint metabolism and address other risk factors in addition to acute inflammation.
Our understanding of osteoarthritis is changing. Osteoarthritis is a chronic disease of the joint and not just purely mechanical wear and tear. This also changes the therapeutic options. A worn-out car tire cannot regenerate, but cartilage damage can. In the case of pronounced mechanical changes that impair the mobility of a joint due to bony growths (lat.: osteophytes) or free joint bodies, surgical treatment makes sense for those affected. Germany is one of the world’s leading countries in the field of joint replacement surgery, i.e. arthroplasty. However, it is very often possible to preserve a joint with cartilage damage. I will explain these options below.
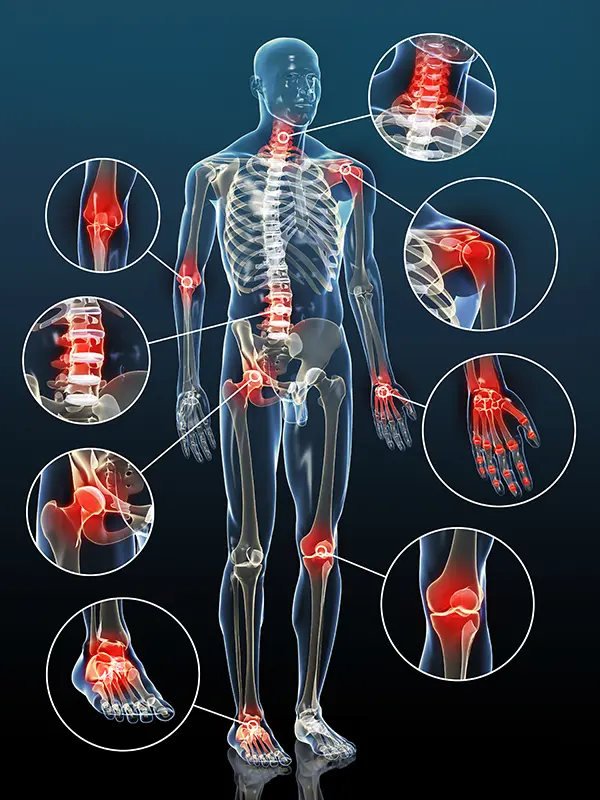

Get to know the guide for patients with joint wear and tear!
What therapies are available?
There are numerous therapy options for the treatment of osteoarthritis. We discuss which measures are sensible and promising as part of a personalized osteoarthritis therapy together at the start of treatment.
In my guide “The osteoarthritis consultation” I explain a holistic concept for your joint health. Those affected have many opportunities to influence the course of their osteoarthritis. Exercise, diet and reducing damaging behavior are just a few examples. On this page, I would like to explain how I can support you medically with joint-preserving therapy.
There are various regenerative therapy methods. We also speak of orthobiological therapies. We use them to exploit the regenerative potential of our body. The aim is to inhibit inflammation, improve joint metabolism and, as a result, reduce pain and improve function. These are primarily hyaluronic acid, the body’s own plasma and regenerative cells from fatty tissue. These are particularly effective due to the stem cells they contain.
What factors influence the choice of therapy and its success?
There are a number of ways to treat osteoarthritis conservatively. The size, depth and localization of the cartilage damage are decisive factors in the treatment decision. These are determined with the help of radiological imaging.
The individual factors of the patient are very important for complaints. These include body weight, training condition, diet, occupational and sporting stress on the joint and the patient’s demands.
Osteoarthritis self-test
As an expert in osteoarthritis therapy, I offer you an image-based osteoarthritis self-test to help you assess your personal risk in just a few steps.
Look at the pictures and add up your points at the end.
What you get out of it: I will show you which signs indicate a possible joint strain. Important: This self-test does not replace a medical diagnosis. If you have severe or persistent symptoms, please make an appointment.
Better results through scientific monitoring of your therapy
The possibilities for treating osteoarthritis are constantly evolving. In order to check the quality of my care and the effectiveness of innovative therapies, I have been scientifically evaluating treatments for many years. To this end, I cooperate with the University of Bielefeld, Charité and the International Cartilage Research Society (ICRS).
I therefore ask my patients to answer a few web-based questions during treatment with Sinogel (hyaluronic acid), stem cells (SVF/ACP) and arthrosamide. The survey is carried out at the time of treatment, after 3, 6 and 9 months and then once a year. Various orthopaedic scores are determined, which cover the areas of pain perception, joint mobility and resilience as well as quality of life.
Patients can register under this link before undergoing orthobiologic treatment of the knee joint.
What treatment options do I have for joint-preserving osteoarthritis therapy?
My aim is to preserve joints rather than replace them. In the case of cartilage damage that cannot be repaired surgically, I primarily use orthobiological substances.
How does treatment work?
The first step is a detailed consultation, a physical examination and an assessment of the radiological imaging. Our own radiologists can produce MRI, CT, DVT or X-ray images at short notice. Appointments can be made in combination with imaging.
Existing images can be uploaded to our practice system in advance via the following link.
If you have to travel a long way, an initial assessment can also be carried out by telephone before SVF / ACP / MFAT (stem cell) therapy, provided that recent images from the last 12 months are uploaded to us.
The severity of the cartilage defect, the joint mobility and the level of pain and your requirements are decisive criteria for the treatment decision. At the end of the consultation, we will decide together how to proceed if you wish to be treated by me.

Cartilage transplantation for osteoarthritis of the knee joint with AutoCart
The treatment is usually performed on an outpatient basis. Anesthesia for SVF / ACP / MFAT is administered locally on the abdomen and the joint. The other injections are preceded by cold therapy of the joint (Cryofos).
This means that you can arrive and depart yourself. For a very long journey of several hours, I recommend an overnight stay on site, at least for SVF / ACP / MFAT therapy.
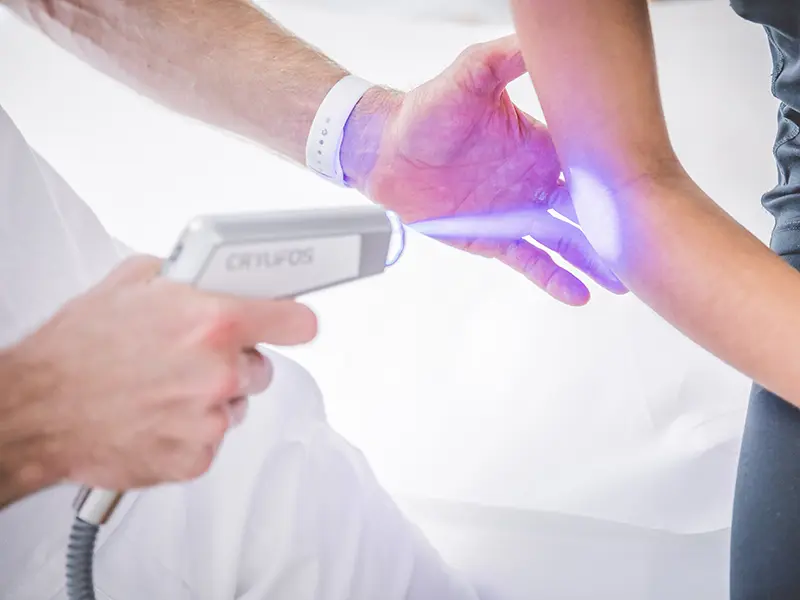
Treatment with cryotherapy (Cryofos)
I usually carry out controlled injections using ultrasound or CT. This ensures that the joint is hit safely. Scientific studies show that injections into joints without imaging often do not achieve their goal. Patients can put weight on their joints immediately after treatment. In some cases, the treated joints may be temporarily painful and feel swollen in the first few days. These symptoms usually subside within the first two weeks. Very physically demanding or unaccustomed strain should be avoided during this time.
In the case of orthobiological treatment with SVF, MFAT, Lipogem, Arthrosamide and IOBP, I recommend resting for the first two weeks after treatment
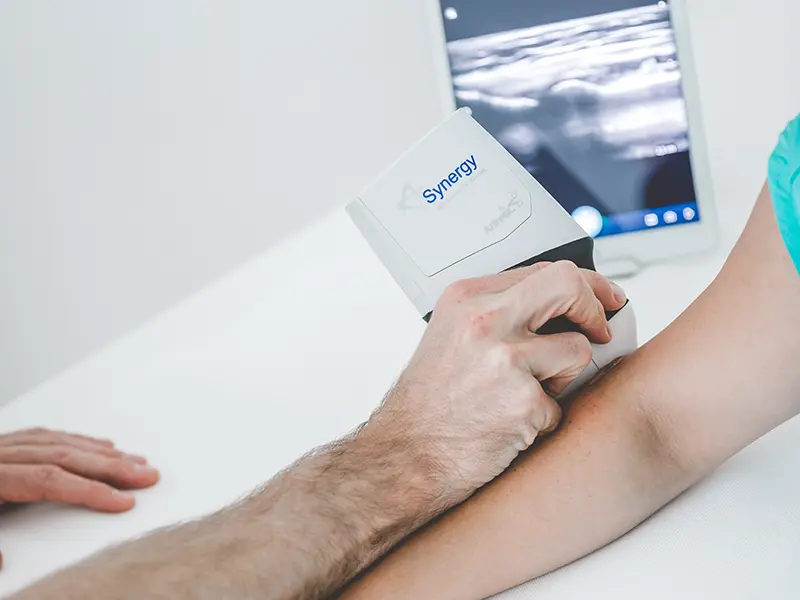
Injection controlled by ultrasound
Here you can find more information on osteoarthritis treatment with the body’s own stem cells:
Do you have any questions or would you like to make an appointment? With pleasure!
Appointments can be made by telephone or e-mail.
If no current images are available, imaging can be combined with the orthopaedic presentation. Existing images and findings can be sent in advance via the following link:
The osteoarthritis consultation by Markus Klingenberg
The osteoarthritis consultation is a guide for patients with joint degeneration.
“Preserving joints instead of replacing them” is the aim of the experienced orthopaedist and sports physician Dr. Markus Klingenberg. The cartilage doctor provides an entertaining overview of the current state of knowledge on osteoarthritis and its treatment options.
Books on Demand
Where can I order the book and audiobook online?
Also available immediately as an audio book!